At Leukoplast, we believe wound healing is a right everybody deserves. We are proud to provide you with a wide range of evidence-based product solutions that you can feel confident in supporting your patients with high-quality care in their wound healing process.
Discover our reliable Leukoplast skin sensitive solutions!
Integrated solutions for better skin tear care
“Skin tears represent more than one in ten wounds in skilled nursing facilities.”1 They are an often-misunderstood issue and can become a serious problem if not treated correctly.
When a skin tear occurs, a comprehensive approach to treatment is required. The selection of wound care products depends on individual patient needs and is crucial for successful wound healing.
Silicone-based dressings allow for atraumatic removal, ensuring that fragile skin is not further harmed. That’s why we recommend you try Leukoplast skin sensitive – a very comprehensive range of silicone-based dressings.

Your complete care solution for skin tears: Leukoplast STEPS
Based on the ISTAP (International Skin Tear Advisory Panel) best practice protocol, Leukoplast STEPS provides easy-to-follow guidance on all aspects of skin tear management, including selecting the correct products for your patients.
Everything at a glance:

Guiding You on Your Educational Journey
Register with PATH to access the latest educational resources that will help you provide the best possible patient care.

Solutions for every stage of skin tear care

Treatment
Ready-to-use products
Products with a soft silicone adhesive cover the special needs of fragile and sensitive skin. Compared to standard adhesives, soft silicone adhesives require less peel force upon removal and enable an atraumatic dressing removal to reduce the risk of adhesive-related skin injuries.
Learn more about Leukoplast® skin sensitive >>
Visit the Cutimed® website >>

Build your own solution
You can also build your own individual solution using silicone adhesives – with the following products.

Recovery
Low levels of compression are recommended for all patients with lower limb skin tears. Products like JOBST® SoSoft and JOBST® Opaque may be suitable.
For patients with venous leg ulcers who have had a full vascular assessment, high compression can be used. Products like JOBST® UlcerCare and JOBST®. Compri2 may be considered.

Prevent
Choosing the right skin care products for individual patient needs is essential for skin tear prevention. "Skin moisturisers aim to repair or strengthen the skin barrier, maintain or increase its water content, reduce trans epidermal water loss (TEWL) and restore or improve the intercellular lipid structure"2.
Products such as Cutimed® ACUTE and TENA® PROskin Body Lotion are specifically designed for sensitive, ageing skin, and they are effective and caring.
All you need to know: Watch our video

Skin tears constituted 41.5 % of known wounds amongst residents (with an average age of 80 years) in a 347-bed Western Australian long-term care facility3.
A skin tear prevention program implemented in a nursing and rehabilitation center with 209 beds in North America reduced the costs for dressings and labor by $1,698 per month4.
Good to know: the basics of skin tears
What are skin tears?

"A traumatic wound caused by mechanical forces, including removal of adhesives. Severity may vary by depth (not extending through the subcutaneous layer)."(5)
- Not to mix up with 'laceration' 5
- Can cause complications, e.g. infections 3,6
- Healing time varies from weeks (acute) to months (complex/chronification) 5

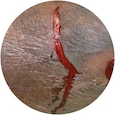
Type l: No skin loss
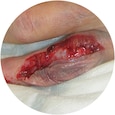
Type ll: Partial flap loss
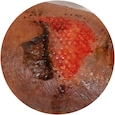
Type lll: Total flap loss
How to treat skin tears?
The ISTAP recommends the following protocol:5
Control bleeding
To stop the bleeding, apply pressure and, if necessary, elevate the limb.

Cleanse and debride
Clean the wound to remove hematoma or residual debris. In case of a necrotic skin flap, it may need to be debrided. Re-approximate the skin flap if it is still viable.

Manage infection
Determine wound infection based on wound assessment signs and symptoms and take appropriate infection control measures. Check the patient's tetanus immunization status.

Monitor wound edge/closure
Skin tears typically close within 14-21 days. Address all factors that could delay healing, such as diabetes, peripheral oedema, etc. Consider compression therapy if the wound is on the lower leg.

Control moisture
Moisture balance is essential to promote wound healing and to protect the peri-wound skin from maceration. Observe the volume and viscosity of the exudate when selecting a topical wound dressing.

Who's at risk?
Certain groups of patients with fragile skin, such as the elderly and newborns, are at a high risk of skin tears. Various intrinsic and extrinsic factors increase the risk of skin tears.
Elderly patients and infants
Patients with frequent dressing changes
Patients with disease-related fragile skin
Patients on certain medications
More information
Leukoplast STEPS wall chart
Your trusty reminder: the most important things to know at a glance.

Learn more from ISTAP
Comprehensive information from the International Skin Tears Advisory Panel.

Contact us
If you would like to know more about Leukoplast skin sensitive, or simply discuss how we can support you in reducing the risk of skin tears, just fill out the form below and one of our dedicated representatives will be in touch shortly.
References
1 Fraser RDJ, et al. Analysis of real-world data from North American skilled nursing facilities’ skin and wound records for skin tear prevalence, healing, and treatment. J Wound Management. 2022;23(2):87-98.
2 Van Tiggelen H, et al. Skin tears anno 2022: An update on definition, epidemiology, classification, aetiology, prevention and treatment. J Wound Management. 2022,23(2):38-51.
3 Stephen-Haynes J, Carville K. Skin tears made easy. Wounds International. 2011;2(4):1–6.
4 Bank D, Nix D. Preventing skin tears in a nursing and rehabilitation center: An interdisciplinary effort. Ostomy Wound Management. 2006; 52(9):38–40.
5 Idensohn P, et al. Skin tears: a case-based and practical overview of prevention, assessment, and management. J Community Health Nurs. 2019;33(2):32–41.

